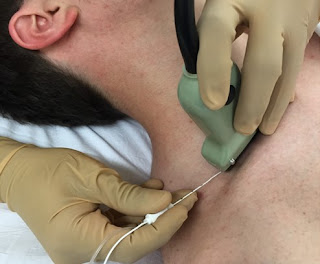
Ultrasound Artifacts
1-Reverberation artifact:
➧ The processing unit in the ultrasound machine assumes echoes return directly to the processor from the point of reflection.
➧ Depth is calculated as D = V × T, where V is the speed of sound in biological tissue and is assumed to be 1,540 m/sec, and T is time.
➧ In a reverberation artifact, the ultrasound waves bounce back and forth between two interfaces (the lumen of the needle) before returning to the transducer.
➧ Since velocity is assumed to be constant at 1,540 m/sec by the processor, the delay in the return of these echoes is interpreted as another structure deep into the needle and hence the multiple hyperechoic lines beneath the block needle (Figure 1).
 |
| Figure 1: Reverberation artifact |
2-Mirror artifact:
➧ A mirror artifact is a type of reverberation artifact.
➧ The ultrasound waves bounce back and forth in the lumen of a large vessel (subclavian artery).
➧ The delay in the time of returning waves to the processor is interpreted by the machine as another vessel distal to the actual vessel (Figure 2).
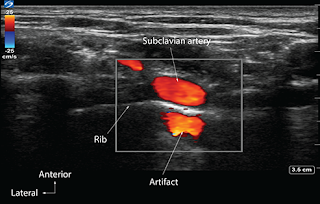 |
| Figure 2: Mirror artifact |
3-Bayonet artifact:
➧ The processor assumes that the ultrasound waves travel at 1,540 m/sec through biological tissue. However, we know that there are slight differences in the speed of ultrasound through different biological tissues.
➧ The delay in the return of echoes from tissue that has a slower transmission speed, coupled with the processor’s assumption that the speed of ultrasound is constant, causes the processor to interpret these later returning echoes from the tip of the needle traveling in tissue with slower transmission speed as being from a deeper structure and thus giving a bayoneted appearance.
➧ If the tip is traveling through tissue that has a faster transmission speed, then the bayoneted portion will appear closer to the transducer (Figure 3).
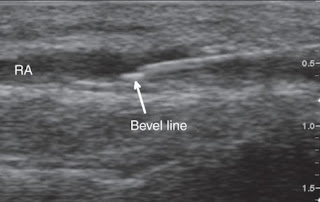 |
| Figure 3: Bayonet artifact |
4-Acoustic Enhancement artifact:
➧ Acoustic enhancement artifacts occur distal to areas where ultrasound waves have traveled through a medium that is a weak attenuator, such as a large blood vessel.
➧ Enhancement artifacts are typically seen distal to the femoral and the axillary artery (Figure 4).
 |
| Figure 4: Acoustic enhancement artifact |
5-Acoustic shadowing:
➧ Tissues with high attenuation coefficients, such as bone, do not allow the passage of ultrasound waves.
➧ Therefore any structure lying behind tissue with a high attenuation coefficient cannot be imaged and will be seen as an anechoic region. (Figure 5).
 |
| Figure 5: Acoustic shadowing artifact |
6-Absent blood flow:
➧The Color-Flow Doppler may not detect blood flow when the ultrasound probe is perpendicular to the direction of blood flow (Figure 6).
➧ A small tilt of the probe away from the perpendicular should visualize the blood flow (Figure 7, Figure 8).
➧ Alternatively, for deep vascular structures, signals may be lost due to attenuation.
➧ Increasing gain, while in Doppler Color-Flow mode, will increase the intensity of the returning signals, which may detect blood flow that was not previously detected.
 |
| Figure 6: Radial a. Absent blood flow artifact |
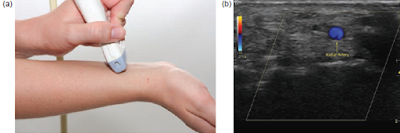 |
| Figure 7: Radial a. Probe tilted away from the direction of blood flow |
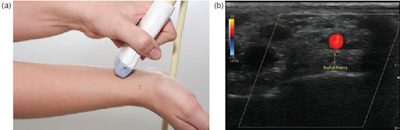 |
| Figure 8: Radial a. Probe tilted towards the direction of blood flow |